Mycobacterium abscessus l,d-Transpeptidases Are Susceptible to Inactivation by Carbapenems and Cephalosporins but Not Penicillins.
Kumar, P., Chauhan, V., Silva, J.R.A., Lameira, J., d'Andrea, F.B., Li, S.G., Ginell, S.L., Freundlich, J.S., Alves, C.N., Bailey, S., Cohen, K.A., Lamichhane, G.(2017) Antimicrob Agents Chemother 61
- PubMed: 28760902 Search on PubMedSearch on PubMed Central
- DOI: https://doi.org/10.1128/AAC.00866-17
- Primary Citation Related Structures:
5UWV - PubMed Abstract:
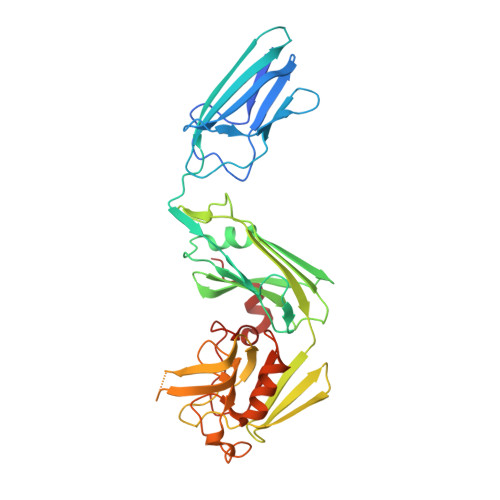
As a growing number of clinical isolates of Mycobacterium abscessus are resistant to most antibiotics, new treatment options that are effective against these drug-resistant strains are desperately needed. The majority of the linkages in the cell wall peptidoglycan of M. abscessus are synthesized by nonclassical transpeptidases, namely, the l,d-transpeptidases. Emerging evidence suggests that these enzymes represent a new molecular vulnerability in this pathogen. Recent studies have demonstrated that inhibition of these enzymes by the carbapenem class of β-lactams determines their activity against Mycobacterium tuberculosis Here, we studied the interactions of β-lactams with two l,d-transpeptidases in M. abscessus , namely, Ldt Mab1 and Ldt Mab2 , and found that both the carbapenem and cephalosporin, but not penicillin, subclasses of β-lactams inhibit these enzymes. Contrary to the commonly held belief that combination therapy with β-lactams is redundant, doripenem and cefdinir exhibit synergy against both pansusceptible M. abscessus and clinical isolates that are resistant to most antibiotics, which suggests that dual-β-lactam therapy has potential for the treatment of M. abscessus Finally, we solved the first crystal structure of an M. abscessus l,d-transpeptidase, Ldt Mab2 , and using substitutions of critical amino acids in the catalytic site and computational simulations, we describe the key molecular interactions between this enzyme and β-lactams, which provide an insight into the molecular basis for the relative efficacy of different β-lactams against M. abscessus .
- Center for Tuberculosis Research, Department of Medicine, Johns Hopkins University, Baltimore, Maryland, USA.
Organizational Affiliation: