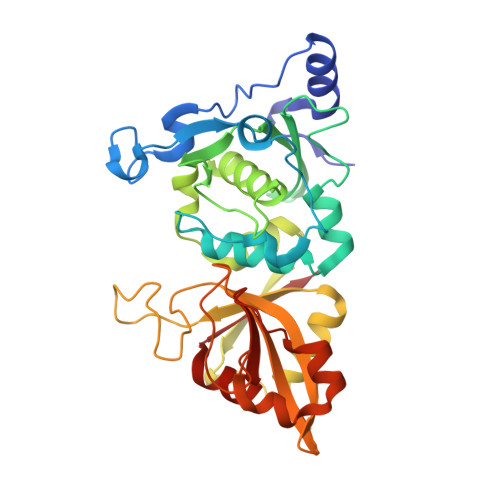
Molecular mode of action of a covalently inhibiting peptidomimetic on the human calpain protease core
Li, Q., Hanzlik, R.P., Weaver, R.F., Schonbrunn, E.(2006) Biochemistry 45: 701-708
- PubMed: 16411745 Search on PubMed
- DOI: https://doi.org/10.1021/bi052077b
- Primary Citation Related Structures:
1ZCM - PubMed Abstract:
Calpain is a nearly ubiquitous Ca2+-activated proteolytic enzyme whose precise physiological function is unknown. However, aberrant Ca2+ homeostasis in the course of cellular injuries and certain diseases of the CNS appears to activate calpain, in turn promoting the degradation of key cytoskeletal and membrane proteins. Hyperactive calpain has also been implicated in various aging phenomena and diseases of late life. Therefore, calpain is considered a potential therapeutic target in preventing degenerations of many kinds. Despite its potential medicinal importance, known structural information about mu-calpain is limited to that from the rat enzyme. We have determined the crystal structure of the human mu-calpain protease core (hmuI-II) containing a Gly213Ala mutation and covalently inactivated by a peptidomimetic (ZLLYCH2F) at 2.0 A resolution. The methylene carbon of the inhibitor is bound to Cys115. Additional hydrogen bonding and hydrophobic interactions between active site residues and the inhibitor, including an intermolecular antiparallel beta-sheet arrangement characteristically observed with members of the papain family of cysteine proteinases, help to stabilize the complex and orient the inhibitor. The terminal ZL portion of the inhibitor is solvent-exposed and highly flexible, and is thus not involved in specific binding interactions with the enzyme. Two large enzyme regions flanking the active site are highly flexible; they may be important in recognition of calpain's natural protein substrates and in positioning them for catalysis. The implications for drug design are discussed.
- Department of Medicinal Chemistry, University of Kansas, Lawrence, Kansas 66045, USA.
Organizational Affiliation: